HIV: Testing ourselves out of the epidemic?
Following the legalisation of HIV home testing in the UK, it will have taken just over a year for the first HIV self-testing kit to become available. The announcement came with the usual hopeful optimism and belief that self testing will make a key contribution to curbing the HIV epidemic in the UK.
Interestingly the kit now available is from an unexpected provider. Where many expected Orasure, here comes BioSure. The device build on a kit previously used by professionals in healthcare settings and was marketed either as the Chembio Sure Check HIV 1/2 Assay or as the Clearview Complete HIV 1/2 Assay. The test is based on the detection of antibodies against HIV using a drop of blood and comes with a 3 months window period (i.e. it does not detect very recent infection).
A simplistic answer to a complex problem
The UK Health Protection Agency (HPA) estimates that 25% of those infected with HIV do not know they are carrying the virus. Further, it is estimated that an overwhelming number of new infections are attributable to those who do not know that they are infected and especially to those who have been recently infected (1).
| “Knowing your HIV status is important. It is possible to reduce or eliminate your risk by making safe and informed choices in your life. The fact is that HIV is preventable.” BioSure Website. |
The reasons for not testing are complex, numerous and intertwined (Box 1). To claim that self testing at home can solve the problem is wishful thinking. To hint that knowing your HIV status can protect you against HIV is misleading (BioSure’s attention has been drawn to this wording).
HIV testing act as gatekeeper allowing those who decide to test to either engage with care if they test positive or to take action to remain uninfected if they test negative. As such, testing is very important and people should be encouraged to test regularly. But in both cases, they are no certainty that those who undergo an HIV test will take either path. Not all those who test positive are ready or willing to start treatment and to keep up with it (2). Not all those who test negative have the will and power to do all what it takes to remain negative. In both cases, attrition is a reality we can’t ignore and something HIV testing can do little about.
| Box 1. Common reasons for not testing (from AIDSMAP) |
|
Perpetuating stigma
Stigma is one of the many barriers to testing though not the only one. Promoting HIV home testing as a discreet option to test, and a comfortable alternative to testing in other settings (which are much more diverse than just clinical settings and include testing in community venues, in GP surgery, in A&E, etc…) only contribute to reinforcing the stigma and fear amongst those who do not take a test for fear of “someone else [having] to know your status.” (BioSure Website) (3).
What happens next once people test positive at home remains a key concern to many including sexual health specialists. If people so fear having to take a test in traditional healthcare settings, how are they going to engage with care at all? Someone else will have to know your status if you test positive.
Facing our fears: Fight Club meets HIV prevention
It is a strange proposition that HIV home testing will “empower people to discreetly test themselves”. Empowerment and discretion are somewhat antithetic. Then what to make of BioSure CEO Brigette Bard claim that home testing is “a significant step towards normalising HIV testing” when the company’s selling point is privacy (4), discretion and not having to talk to other about it.
The reality is that many people have few issues with testing in healthcare settings. Testing rates have been increasing year-on-year with more than a million tests performed each year and this across communities, including those who are most affected. A 2014 Survey conducted amongst Black African in the UK have shown that when asked to consider where they would like to take an HIV test in the future, most people who had already taken a test name a GP surgery. HIV home testing kits (with an immediate result) was the most preferred setting among those who had never tested (we go back to fear and stigma).
| ““We needed to get more people tested and find undiagnosed cases so they can get access to treatment, but we need to try to help ensure that people are able to access the right support and know what is available.” Stacey Adams, sexual health manager at the Manchester-based LGBT Foundation |
This may indicate a role for HIV home testing for those who have never tested but it also shows that once people have taken a test they are fine with it being done in healthcare settings where they can be linked to care, as well as being tested for other STIs which contribute to the spread of HIV. It also suggests that self testing will foster stigma rather than address it. Get people to test once, do it properly, and they will come back.
The same survey showed some stunning findings (Box 2) which just confirmed that the problems faced by HIV prevention are much deeper than what self-testing can address and that other interventions are urgently needed to address sociocultural issues.
| Box 2 – Some key finding of the 2014 survey of Black African in the UK that Home testing does not address. |
|
Clearly, people’s experience when going for an HIV test in clinical settings can make or break the intervention. In a piece for Vice Tom Hayes relates his shocking experience of testing in an NHS clinic.
Tom tested before going on holiday and when his results came back and the clinic tried to get in touch with him, he was told “Fuck… Don’t have sex with anyone and call us as soon as you get back.”
The experience deeply unsettled him, “For weeks I ignored the calls, texts, and letters from the HIV clinic urging me to come in for my initial appointment after the diagnosis” he writes.
Could this also describe someone’s reaction to a positive home test? With nobody to talk to, not even the strength to pick up the phone, and no one to chase you, what would you do next?
Will the HIV home-testing kits be an invaluable asset “For those who feel physically or mentally unable to go to a clinic”, as Tom thinks? Or will it just take them one step further away from care?
Of course, those who do not have such physical and mental issues could benefit from home testing, but these are not the problem. Then why would they opt for a £29.95 option when testing in professional settings is free and use a better testing technology than what BioSure offers?
Again, instead of addressing structural problems, many of which are key contributors to the epidemic, we just throw a new toy in the pram, hoping it will make a difference.
Beyond the headline, HIV prevention on the line
The Health and Social Care Act 2012 introduced a dramatic change in how HIV prevention and care are managed. Put simply the act decoupled prevention from treatment and care services, devolving prevention to local health authorities, up to them to decide how much is worth investing in an area of health often controversial (after all, people can just use condoms, that’s in line with 30 years of HIV prevention messaging that still resonates for many, even among the most affected communities e.g. gay men)
Rolling out HIV self testing at home is going one step further; it is disconnecting the gatekeeper from the path to prevention and care.
Whilst we are discussing the pro and cons of a gimmick intervention that provides the government and Public Health bodies an opportunity to window-dress their HIV prevention effort, it creates a diversion from the real issues at stake: decreased funding for HIV prevention, increasing burden on GUM clinics to do more with less (which may explain bad testing experience), and shifting responsibility and cost of testing to the people at risk. After all, tests are now available, easy to use, discretely, from the comfort of your home.
No magic bullet (and other truisms)
That no one solution fits all or that no one tool will work for everyone are becoming tiresome truisms. Yes, we need a range of tools and options and interventions, so why it is that HIV prevention in the UK is building on two pillars: HIV testing and condoms? What happens to other options which we know work but remain unavailable (I can’t but mention PrEP)? Or to interventions that address broader issues such as mental health, employment, drug use? Where are the holistic HIV prevention interventions? What happened to well-being, to health which encompasses and is affected by so many other issues?
Imagine public health was managing contraception as it does HIV prevention. Imagine a world where contraception would be limited to two interventions promoted and endorsed by public health: one promoting the pill, the other promoting abstinence, one promoted on even years, the other on odd years. Does that strike a chord?
Years after years and campaigns after campaigns, condoms and testing have become iconic symbols of prevention, to the point that an HIV specialist describes testing as the “single biggest thing that we can do to have a major impact on the HIV epidemic”. This flies in the face of data showing that despite increased testing rates (and with a rate of condom use remaining about constant) the rate of new infections has remained constant for the past decade. Uptake of the Orasure test, which has been available in the US since 2012, has remained limited and did not change the face of the epidemic.
| “The single biggest thing that we can do to have a major impact on the HIV epidemic is to dramatically increase HIV testing rates, especially in those most at risk. The availability of HIV self-testing will help us achieve that.” Dr Michael Brady Kings College Hospital NHS Foundation Trust |
Who is testing, and who is not, and how often are more important questions. Whether HIV home testing will reach those who currently do not test for reasons other than comfort and discretion remains unknown but could be/have been investigated prior to changing the legislation and would have helped with the roll out (again, PrEP was put on trial, not home testing).
HIV testing is a critical component of a comprehensive HIV prevention strategy. Dr Brady pointed (via Twitter) to a mathematical model showing how much testing could impact the epidemic (Prof, Andrew Phillips, UCL). This is a great model, which relies on two big “IFs”: the first is uptake of testing (any testing), the second is linkage to care and rapid initiation of treatment. The second “IF” is a big challenge for people who are not testing in conventional healthcare testing.
Like the Test and Treat model presented by Reuben Granich in 2009, Philips model tells you what the intervention could do, not how to deliver it, or how best to deliver it (5). These are public health policies to be worked out with the involvement of the community (which rarely happen). Another model by David Katz that looked specifically at the impact of self testing has showed a potential negative effect on the course of the epidemic if self testing was to replace standard testing.
Is there still a rational for such a reductionist approach to HIV prevention? Altogether, despite regular growing testing rate, the intervention seems to have reached a plateau and is failing to reach those who needs to be reached. Doing more of the same may not be the best public health policy we could come up with.
There is so much more to do that could make a real impact on the course of the epidemic. The focus on a limited number of interventions is puzzling. We could start by implementing existing guidelines and broadening testing to various contexts and doing it better. Some have called for years for an opt-out approach to testing in the NHS, GPs are failing and reluctant to offer testing to patients who would benefit from it (6), sex education is still found wanting, and the list goes on.
As Deborah Gold, chief executive of the National Aids Trust (NAT) said: “We currently have a long way to go when it comes to diagnosing people with HIV on time.” On time and at home are not one and the same thing. And as much as we can’t just treat ourselves out of the epidemic, we just can’t test ourselves out of the epidemic.
~rjt
Further readings:
- Self-testing for HIV and its impact on public health – Sex Transm Dis. PMC 2015 Jan 1.
- HIV testing. Aidsmap
(1) Which makes the length of the window period an important factor when deciding which test to go for.
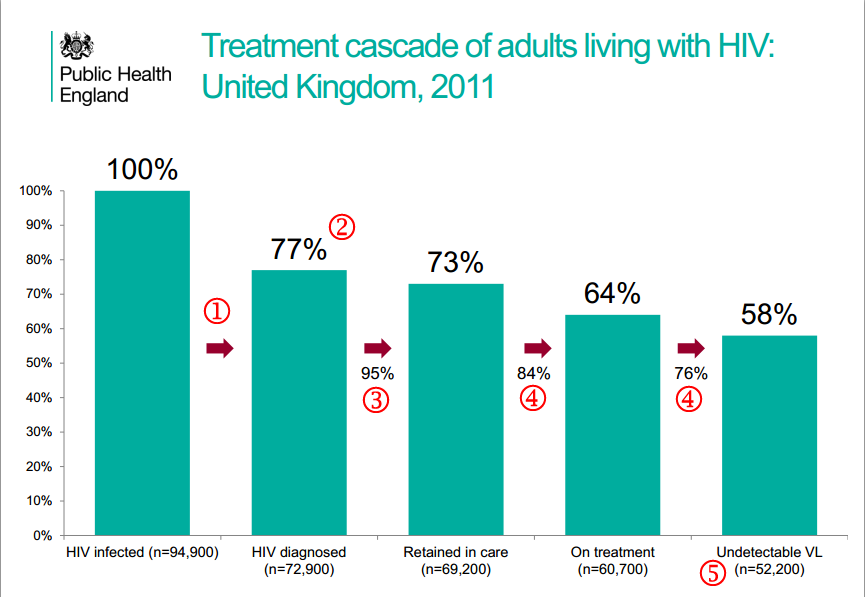
(2) The UK “cascade of care” is remarkably good. 97% of people newly diagnosed with HIV were connected with specialist care within three months, and 95% of people who attended during one year were retained in care the following year. Few other countries have comparable results. HIV self testing could challenge this success.
(3) Lest we forget, HIV testing in the UK is free, voluntary and confidential.
(4) Privacy is a big thing but the BioSure website is rather silent about what it does with the name and address of those who order a test online.
(5) Published in 2009, the Granich model made the bold claim that Test and Treat “could greatly accelerate the transition from the present endemic phase, in which most adults living with HIV are not receiving ART, to an elimination phase, in which most are on ART, within 5 years. It could reduce HIV incidence and mortality to less than one case per 1000 people per year by 2016”. As we reach 2016, we are far from such bold results, for many reasons the model was not looking at.
(6) Recent studies showed that training general practices to offer rapid HIV tests leads to increased detection and earlier diagnosis of patients with HIV infection.